In the bustling medical corridors of Western New York, from the specialized clinics in downtown Buffalo to the primary care offices in our suburban neighborhoods, a troubling pattern is emerging. Many local patients report leaving their appointments feeling ignored, as if their physical pain was merely a product of their imagination. This phenomenon, known as medical gaslighting, is more than just a communication breakdown; it is a systemic issue that leads to missed diagnoses and delayed care, often with devastating consequences for our community members.
Understanding the Layers of Medical Gaslighting
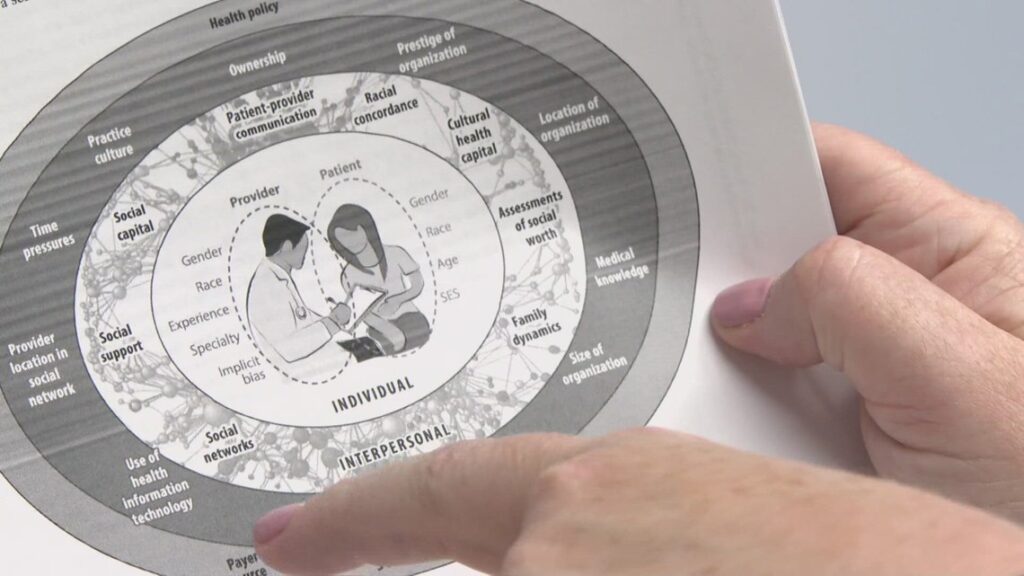
Dr. Karen Spencer, a veteran researcher who has spent decades analyzing patient-provider interactions, describes medical gaslighting as a multi-layered experience. It occurs when a patient’s reported symptoms are dismissed, minimized, or attributed to psychological factors without proper investigation. Dr. Spencer likens the issue to “layers of an onion,” where the core interaction is influenced by the surrounding organizational culture and broader health policies.
For many in the Buffalo-Niagara region, this manifests as feeling “unseen and unheard,” often being sent home without a diagnostic plan while their symptoms continue to escalate. This invalidation can cause patients to doubt their own physical sensations, further delaying the search for necessary treatment.
The Systemic Pressures on Western New York Care
While it is easy to point fingers at individual practitioners, the reality is often rooted in systemic strain. Healthcare providers across Erie County are navigating a landscape where they are required to see upwards of 17 patients in a single shift, often with limited administrative support. These time constraints can lead to “tunnel vision,” where doctors focus on the most obvious symptoms rather than the complex, underlying issues reported by the patient.
Furthermore, historical bias in medical training continues to play a significant role. For decades, clinical research was primarily conducted on male subjects, leading to a “one-size-fits-all” approach to medicine. Dr. Spencer notes that this bias often results in the dismissal of patients whose physiological presentations do not fit the traditional—and often outdated—medical textbooks.

Vulnerable Populations and Local Disparities
At the Lake Erie Times, our reporting frequently highlights disparities in local healthcare outcomes. Medical gaslighting disproportionately impacts women, people of color, and trans patients. These groups are more likely to have their physical pain misattributed to anxiety or emotional distress.
Common examples include women being advised to “simply relax” or “take a bath” in response to chronic pain, or patients being offered antidepressants when their emotional frustration is actually a logical reaction to being ignored by the medical system. Dr. Spencer has observed these dynamics even within her own family’s experience with cancer, proving that professional knowledge does not always shield one from being dismissed.
Strategies for Patient Advocacy
Navigating the healthcare systems in Buffalo requires a proactive approach. To ensure your concerns are taken seriously, consider the following strategies for your next appointment:
| Advocacy Step | Action Plan |
|---|---|
| Preparation | Track symptoms in a journal and submit questions via patient portals before the visit. |
| Documentation | Request that any refused tests or treatments be explicitly noted in your medical record. |
| Support | Bring a trusted friend or family member to serve as a witness and second set of ears. |
| Second Opinions | If a provider is not a fit, seek a consultation with a different specialist immediately. |
Be Your Own “CEO”
Dr. Spencer advises patients to “be the CEO of your own healthcare.” This means arriving with a clear agenda and not settling for vague answers. “If you’ve been tracking symptoms, write that down and bring it with you,” she suggests. By providing data, you make it more difficult for a provider to dismiss your experience as purely subjective.

The Power of a Support Person
In many Western New York practices, having an advocate in the room can shift the power dynamic. A support person can take detailed notes, ask clarifying questions, and provide emotional backing if the provider becomes dismissive. This ensures that the patient’s narrative remains the focus of the consultation.
A Path Forward
If you feel your medical concerns are being sidelined, remember that you are not alone in this struggle. Local resources and patient advocacy groups are available to help Western New Yorkers navigate these challenges. As Dr. Spencer emphasizes, “You’re not crazy. Don’t give up.”
For those looking for a deeper dive into navigating the complexities of the modern healthcare system, Dr. Karen Spencer’s upcoming book, Your Good Death: Why End-of-Life Healthcare is so Difficult and How to Make it Work for You, offers critical insights into advocating for yourself and your loved ones during the most vulnerable moments of care.
Disclaimer: The content provided by Lake Erie Times is for informational purposes only and should not be considered as professional medical, legal, or financial advice.
Affiliate Disclaimer: Some links on Lake Erie Times are affiliate links. This means that if you make a purchase through these links, we may earn a commission at no additional cost to you. Our recommendations are based on careful research and our commitment to quality journalism.